
What Causes Dental Anxiety and How to Overcome It
As you are skimming through your calendar, you fill with dread as you notice that your six month dental appointment is coming up. With each

As you are skimming through your calendar, you fill with dread as you notice that your six month dental appointment is coming up. With each

Everyone has heard about cavities. We also all know that we are supposed to brush our teeth twice a day and floss once a day

Regular dental care is important for everyone, but it can be especially important if you are an expecting mother. Did you know that your dental

Patients have questions, so we provided this page with the hopes that it answers some of the questions you may have! There are plenty of
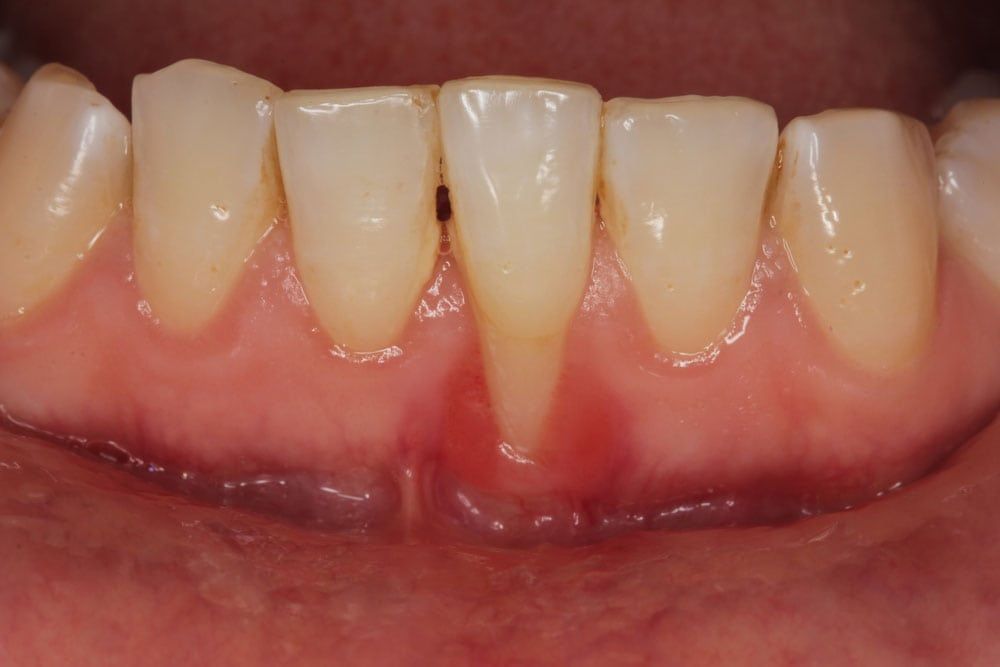
Treating Gum Disease Your gum disease treatment will depend on several factors, including your personal health history and the stage of your gum disease. This

Healthy Mouth, Healthy Body – Making the Connection Your mouth is a window into the health of your body Insight about your overall health can
Periodontal disease is also known as gum disease Periodontal (perry-o-DON-tal) Disease is an infection and inflammation that affects the tissues and bone that support your teeth.

With good oral care at home and regular dental visits, children can reach adulthood without suffering from tooth decay and other oral health problems. Diet
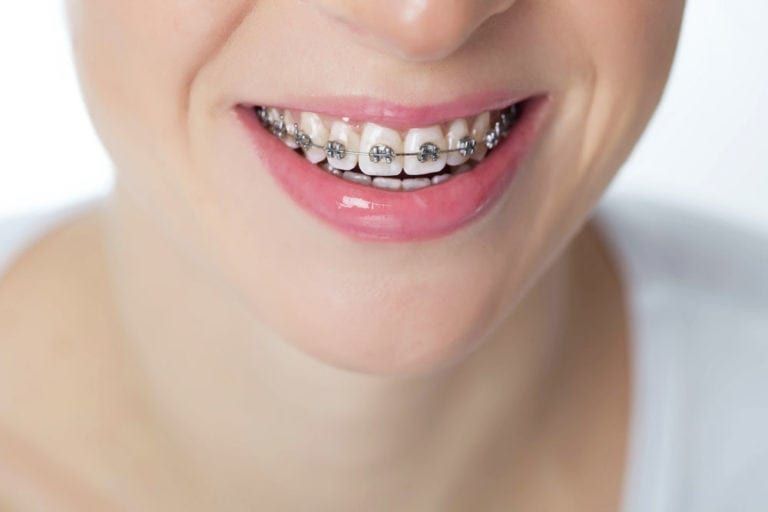
Crooked teeth and bite problems are often solved with orthodontic treatment. Sometimes, even when teeth look straight, the upper and lower teeth may not fit